|
Persaud stressed the significance of the fact this person identifies as mixed race. “What all of these individuals have in common is that their cancer-treating physicians looked specifically for these HIV-resistant cells to get to cures for two diseases, with having to replace their immune system because of their blood cancers with the new one that is resistant to HIV,” she said. Persaud added that “the haplo-cord approach with HIV-resistant cord cells is feasible in adults living with HIV” and the “less stringent” matching process for cord cells makes this process “more available for racially diverse populations.” She received the transplant at Weill Cornell Medicine in 2017. To rectify this, the researchers used CCR5-delta32/32-carrying stem cells from umbilical cord blood to cure her cancer, and, ultimately, HIV. As a result, it is incredibly hard to find stem cell donor matches for people of color being treated for these blood cancers. Roughly 1% of white people have this mutation and it is even rarer in non-white populations, according to a press release. The presence of this mutation means these people don’t have the CCR5 receptor that’s needed for HIV to enter and infect a cell. Their matched donors had to possess two copies of the CCR5-delta32 mutation. What unites these different cases is the fact that they all received stem cell transplants for their cancer treatments by way of compatible adult donors. Last year, it was announced a 66-year-old man living with HIV and leukemia – “the City of Hope patient” – had achieved long-term remission from both diseases as a result of stem cell treatments. Since then, he was followed by the “London patient,” Adam Castillejo, and “the Düsseldorf patient,” whose identity has not been revealed. He would die in 2020 when his leukemia returned. Over a decade ago, Timothy Ray Brown, or “ the Berlin patient” was the first person to essentially be cured of HIV by way of stem cell transplants.  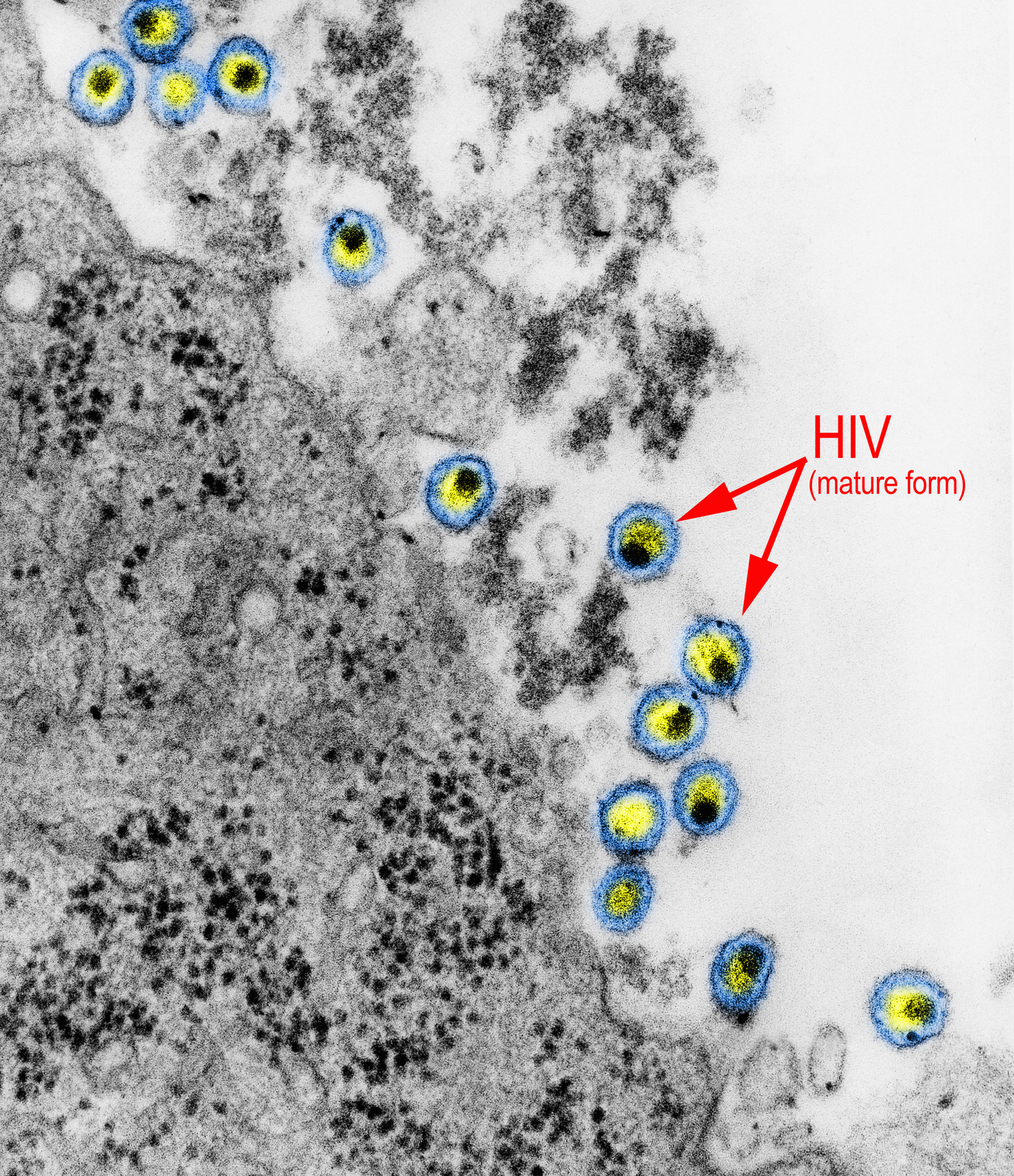
Why this case is a breakthrough in HIV treatment “Just as these three men provide hope for those living with HIV, so does our case, and especially for women.” 
Women represent approximately 50% of people living with HIV globally,” Persaud told Healthline. “This individual is the first woman to be in remission following stem cell transplant for blood cancer. Deborah Persaud, co-lead study author and the interim director of Pediatric Infectious Diseases, and a professor of pediatrics at Johns Hopkins University School of Medicine, said this point is especially important. Given that this is the first woman of color who has achieved HIV remission, experts say it also underscores why more needs to be done to include people from underrepresented communities in studies, clinical trials, and cutting-edge research.ĭr. This case study underscores our growing understanding of how modern medicine is tackling an enduring global health crisis – 38.4 million people are living with HIV worldwide, according to current data from the World Health Organization (WHO). Their stem cell transplants came from compatible adult donors, while hers were derived from cord blood. She follows three others (all men), who have seen their HIV effectively be “cured” as a result of stem cell transplants. They paint a full picture of the so-called “New York patient,” a middle-aged woman who self-identifies as mixed race and has now been living with her HIV in remission since 2017. Now a year later, the researchers are sharing their full findings in the journal Cell. Researchers at the 29th annual Conference on Retroviruses and Opportunistic Infections announced in 2022 that the fourth person was effectively “cured” of HIV by way of stem cell transplants for blood cancer, in this case, acute myeloid leukemia (AML). Previous procedures used stem cell transplants that came from compatible adult donors. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
